
Struggling with itchy, irritated skin and wondering what’s causing your eczema? You’re not alone. Eczema can flare up suddenly—and often without an obvious reason.
At OC MedDerm in Irvine, CA, Dr. Parvin Shafa, bringing over 25 years of dermatology experience across California, helps patients identify the root causes and triggers of eczema so they can better control flare-ups and maintain healthy skin long term.
This guide explains what causes eczema, common triggers, and how to prevent flare-ups.
What Is Eczema?
Eczema (also known as atopic dermatitis) is a chronic inflammatory skin condition that causes:
- Dry skin
- Redness
- Itching
- Irritation
It’s not contagious, but it can be persistent and uncomfortable if not properly managed.
What Causes Eczema?
Eczema doesn’t have a single cause. Instead, it develops due to a combination of:
1. Genetics
If eczema, asthma, or allergies run in your family, you’re more likely to develop eczema.
This is linked to a weakened skin barrier that struggles to retain moisture and protect against irritants.
2. Skin Barrier Dysfunction
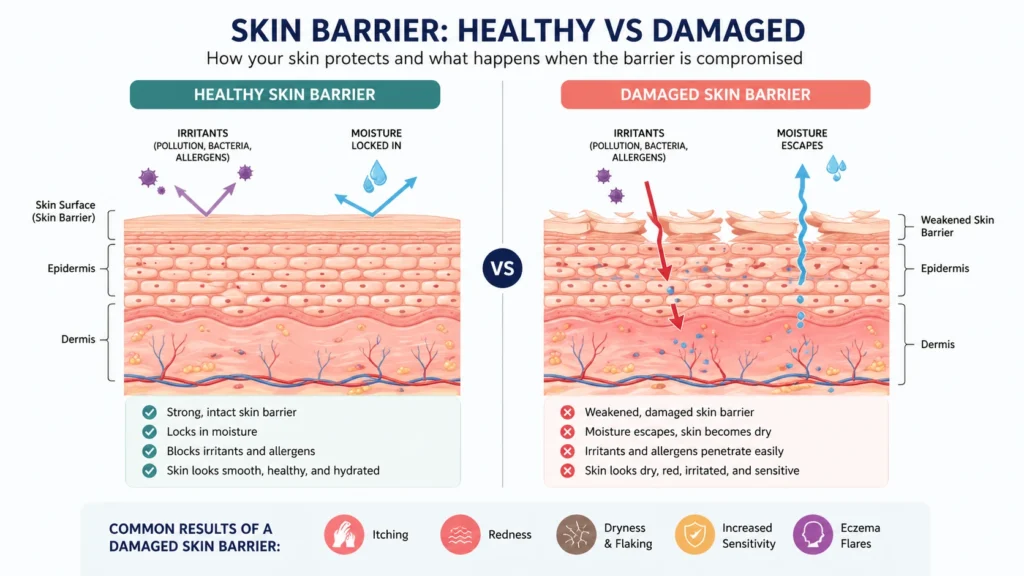
People with eczema often have a compromised skin barrier, meaning:
- Moisture escapes easily
- Irritants enter more easily
This leads to dryness and inflammation.
3. Immune System Response
The immune system overreacts to triggers, causing inflammation in the skin.
4. Environmental Factors
External elements can trigger flare-ups, even if they aren’t the root cause.
Common Eczema Triggers
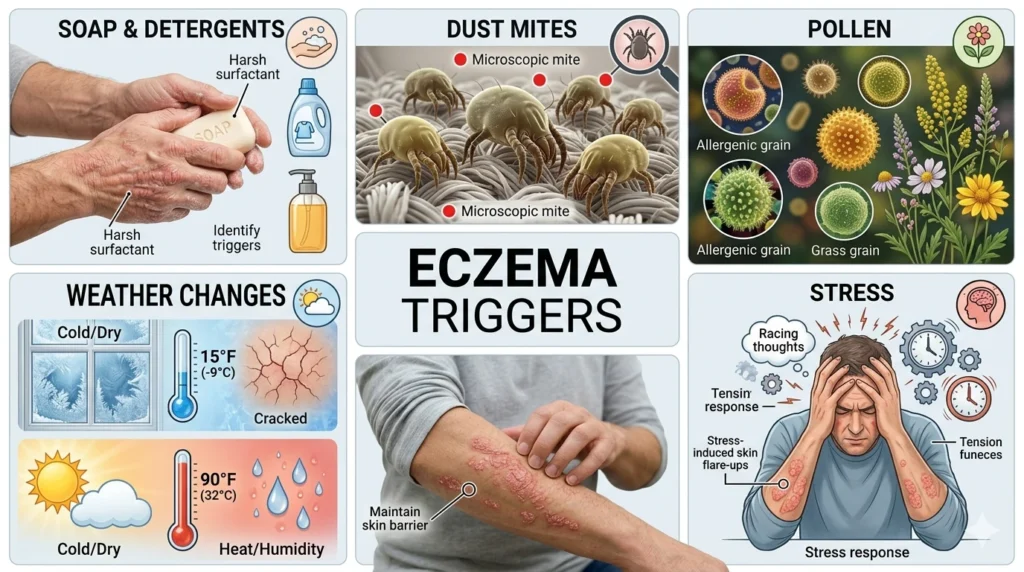
Understanding triggers is key to preventing flare-ups.
Irritants
- Soaps and body washes
- Detergents
- Fragrances
- Cleaning products
These strip natural oils from the skin.
Allergens
- Dust mites
- Pet dander
- Pollen
- Mold
Weather Changes
- Cold, dry air (winter eczema)
- Heat and sweating
Fabrics & Clothing
- Wool
- Synthetic fabrics
- Tight clothing
Stress
Emotional stress can trigger or worsen eczema flare-ups.
Food Triggers (in some people)
More common in children than adults.
Infections
Bacterial or viral infections can worsen eczema symptoms.
Why Does Eczema Flare Up Suddenly?
Even if your eczema is under control, flare-ups can happen when:
- You’re exposed to a trigger
- Your skin becomes too dry
- Your immune system reacts
Often, it’s a combination of factors—not just one.
Where Does Eczema Commonly Appear?
Eczema can affect different areas depending on age:
- Infants: Face and cheeks
- Children: Elbows and knees
- Adults: Hands, neck, face
How to Prevent Eczema Flare-Ups
Keep Skin Moisturized
Use fragrance-free moisturizers daily.
Avoid Known Triggers
Identify and eliminate irritants or allergens.
Use Gentle Skincare Products
Choose products designed for sensitive skin.
Manage Stress
Stress reduction can help prevent flare-ups.
Wear Breathable Fabrics
Opt for cotton and loose-fitting clothing.
When to See a Dermatologist
You should seek expert care if:
- Eczema is severe or spreading
- Over-the-counter treatments aren’t working
- Skin becomes infected
- Flare-ups are frequent
At OC MedDerm in Irvine, CA, we provide:
- Personalized eczema treatment plans
- Advanced therapies for chronic eczema
- Guidance to identify triggers
Treatment Options for Eczema
Depending on severity, treatment may include:
- Prescription creams
- Anti-inflammatory medications
- Moisturizing therapies
- Lifestyle modifications
Final Thoughts
A combination of genetics, skin barrier issues, and environmental triggers causes eczema. While it can’t always be cured, understanding what causes your flare-ups is the key to controlling them.
With the right care and guidance, you can significantly reduce symptoms and improve your skin health.
FAQs
What is the main cause of eczema?
There isn’t one single cause—eczema is influenced by genetics, immune response, and environmental triggers.
What triggers eczema the most?
Common triggers include dry skin, irritants, allergens, and stress.
Can eczema go away on its own?
Mild cases may improve, but many people need ongoing management.
Is eczema genetic?
Yes, it often runs in families.
Eczema Treatment in Irvine, CA
If you’re dealing with persistent eczema or frequent flare-ups, OC MedDerm can help you find the cause and create a personalized treatment plan.
Contact us to schedule your consultation today for expert care.





